Managing Alzheimer’s Patients that Wander
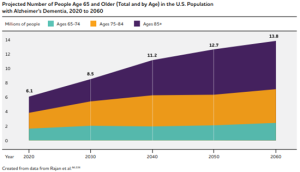
Alzheimer’s is the leading cause of disability and poor health (morbidity) in older adults. And it is only going to get worse. Projections show that the number of people living with Alzheimer’s in the U.S. population is expected to double by 2060 to 13.8 million people aged 65+. As the number of people with Alzheimer’s increases, so does the need for proper care and wander management.
One of the special areas of concern, in people with Alzheimer’s dementia, is the prevention of wandering and wander management. Wandering, also known as elopement, allows for individuals to become lost, putting them at significant risk of injury and death.
What is the distinction between Alzheimer’s and dementia?
Alzheimer’s and dementia are not the same, even though people use the terms interchangeably. There exists a major distinction between Alzheimer’s and dementia. Alzheimer’s is a type of brain disease, while dementia is a classification of a broad range of symptoms. Alzheimer’s disease is one of, but not always the sole cause of dementia. While dementia has several and often mixed causes.
Alzheimer’s Dementia
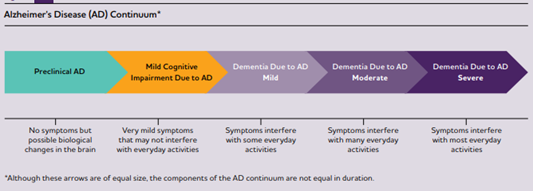
In truth, having Alzheimer’s is not a normal part of aging. Alzheimer’s disease is a type of brain disease that is caused by damage to nerve cells (neurons) in the brain. The first, neurons damaged are those that control memory, language, and thinking. So, problems with these neurons also are cause problems with memory, language, and thinking. These symptoms are hallmarks of Alzheimer’s disease.
The development of Alzheimer’s takes substantial time. By the time symptoms are noticeable, changes to the brain begin 20 years or more before recognized. Nevertheless, Alzheimer’s progression cannot be reversed and can only be delayed. Unfortunately, there is no cure that exists.
Today, a physician can diagnose Alzheimer’s disease with 90% accuracy. However, new research show promises that blood tests and retinal tests can diagnose Alzheimer’s.
Still to this day, however, a confirmed diagnosis is only achieved in one, singular gruesome way. Only upon post-mortem brain examination is Alzheimer’s confirmed. Analysis needs to find the accumulation of protein fragment beta-amyloid plaques, outside of neurons, and the accumulation of abnormal forms of the protein tau inside neurons.
Dementia
Many people with dementia have brain changes associated with multiple dementia subtypes. These causes include Alzheimer’s, cerebrovascular disease, Lewy body disease, frontotemporal lobar degeneration, Parkinson’s, hippocampal sclerosis, and other mixed pathologies.
Mixed Dementia and Alzheimer’s
A mixed dementia diagnosis happens when people have dementia caused by more than one type of brain change. Studies suggest that mixed dementia is the norm, and the number of distinct combinations of mixed dementia is extensive.
The majority of people with the brain changes of Alzheimer’s also have the brain changes of a second cause of dementia. Only 3% had Alzheimer’s disease alone, 15% had brain changes of a different cause of dementia, and a whopping 82% had the brain changes of Alzheimer’s plus at least one other cause of dementia.
Modifiable Risk Factors and Treatment Options
While age, genetics, and family history indicate mental decline and dementia, some risk factors are modifiable to reduce and delay development. Examples of modifiable risks factors include staying physical activity, smoking cessation, continued and higher education, staying socially and mentally active, and maintaining a healthy blood pressure and diet. The Lancet Commission on dementia prevention, intervention, and care suggest that addressing modifiable risk factors might prevent or delay up to 40% of dementia cases. Surprisingly, a new study links drinking 2-4 cups of tea a day to a decreased risk of developing dementia.
Currently, there are 6 FDA approved medications on the market and other non-drug options. Five of the available medications treat only the symptoms of Alzheimer’s, while one medication aims to reduce one of the causes (beta-amyloid plaques). Non-drug therapies include cognitive stimulation, music-based therapy, and cognitive behavioral therapy. These non-drug therapies show promise and are the most typical intervention for agitation and aggression as they are more effective than pharmacologic avenues.
What is wandering and are there any benefits?
Wandering also referred to as elopement, is believed to be a behavioral expression of a basic human need. These include the need for physical activity, social contact and in response to environmental irritants, physical discomforts, or psychological distress. Wandering is a double-edged sword. In some ways, wandering can be both detrimental and beneficial.
The Alzheimer’s Associations provides recommendation that encourage healthy wandering and prevent dangerous wandering. Their recommendations include, facilitating healthy wandering while addressing unmet needs to lessen unsafe wandering.
Negative and Ethically Concerning Wander Management and Prevention
Additionally, some caregivers try to implement ethically concerning control methods that are questionable. Questionable methods include chemical and physical restraints.
Irrefutably, confining and physically restraining those who wander are misguided attempts at curbing the behavior. The use of physical restraint is linked with various negative consequences. These include decreased circulation, physical deconditioning, and mental distress.
With this in mind, every step made to protect those who wander and encourage positive ways and methods to manage wandering are encouraged.
Encouraging Positive Wandering
There exist creative and individually tailored strategies that combat wandering. Caregivers should make every effort to balance the safety and autonomy of the cognitively impaired while also implementing technology that maintains their dignity as individuals.
Caregivers enabling someone to move about safely and independently is recommended. This encourages, supports, and maintains a resident’s mobility and choice. Identifying why wandering occurs helps address unmet needs, prevent unsafe wandering, and successful exit seeking.
Above all, care goals should include encouraging, supporting, and maintaining a resident’s mobility and choice, to enable them to move about safely and independently.
Benefits of Wandering
If done safely, wandering itself is not a problem. Wandering helps relieve stress and boredom, and is good exercise. Benefits of wandering include promotion of circulation and oxygenation, cardiovascular health, and decreased contractures. Also, supported wandering gives a sense of autonomy, reduces aggression and promotes independence.
Wander Management at Home
Many individuals who wander at home put themselves at serious risk of falls and death. However, there are many ways to allow the person to wander and be safe. Just like having an evacuation plan, you should plan for an unsafe wandering event.
Homes preparation is key. Place alarms, locks, and motion-sensing devices to alert when an aging relative moves unsupervised. Low-tech options include attaching bells to doors, child-proof covers on doorknobs, fencing the yard, using hedges to block line of sight, and installing sliding bolts above eye level.
Another way to manage wandering at home is addressing the causes of wandering. Wandering is often the result of everyday activities, emotional stressors, and physical decline.
Regarding everyday activities, caretakers should understand that their relatives may be following past routines, searching for something, trying to get back “home,” or attempting former chores or responsibilities.
Emotional stressors management includes lessening stressors or fear, preventing overstimulation that leads to anxiety, and managing frustration through communication.
Lessening physical discomfort is another manageable stressor. These include hunger, thirst, and the need to use the bathroom. Also, the regulating the temperature of their space and preventing boredom.
Wander Management in Senior Living
Some studies examined the effects of enhanced facility environments and walking programs on nursing home residents. Both studies found beneficial outcomes.
One study evaluated the construction of two scenes with one homelike environment and one with pictures, sounds and smells of nature. The study found that participants spent significantly more time near the two scenes than in the corridors of the facility. However, their pacing did not decline, showing that wanders tend to prefer wandering in those environments.
Also, another study examined the effects of a regular, early-evening walk. The study found a 30% reduction in incidents of aggression in the 24 hours following the walking program.
These studies provide evidence that the creation of soothing environments and activity programs promotes a positive outlet for those who wander.
Technological Options Used for Wander Management
Today there exist technological options to help prevent unsafe wandering, while also promoting perceived autonomy without ethical issues. Electronic devices allow some freedom, reducing the need for chemical and physical restraints. When used correctly, tagging and tracking devices reduce the risk of elopement and also the burden on caregivers.
These electronic devices help balance the safety and autonomy of residents and maintains their dignity as individuals.
Costs of Not Addressing Wandering
When proper mitigation efforts are not in place, the effects of wandering affect more than just the lives of the individual. Facilities across the nation are being fined by state surveyors and litigated out of existence. For instance, 10% of all litigation against long term care facilities involve an elopement.
Furthermore, one such case in Delaware resulted in a jury awarding $18 million in damages. Not all cases make it to trial and out-of-court, and the average settlement is about $400,000.
Wander Management Solutions from RF Technologies
RF Technologies (RFT) provides CODE ALERT Wander Management Solution to safely monitor residents at risk of wandering.
Wander Management keeps patients safe and secure. It prevents elopement while also alerting staff when residents loiter at doorways. The system reduces liabilities and injuries that result from wandering episodes. Preventing the loss of a residents maintains day-to-day calm and a friendly environment for residents and staff.
CODE ALERT Wander Management Solution Technology
CODE ALERT Wander Management Solution is a reliable, comprehensive system for wander management. With customization, RFT accommodates any facilities’ unique needs.
In addition, CODE ALERT features a small, lightweight transmitter, worn on the wrist that mimics a wristwatch. The discrete tagging system helps prevent unsafe wandering while supporting caregiver workflow and helps foster a beneficial home-like environment.

How CODE ALERT Works
Whenever a resident loiters near a door, the RFT system alerts caregivers of the resident and their location. This allows the caregiver to quickly respond and redirect the resident.
Enterprise Software supports CODE ALERT and fully integrates wander management and nurse call on a single platform. Staff are alerted from anywhere and respond to the alarm as alerts are pushed to tablets and mobile phones through the RFT Cares App.
Enterprise Quality Dashboard Module
The RFT Quality Dashboard Module supports data from Enterprise Software. This module is an optional tool that offers reporting and analytics. Data gleaned from the module helps identify the true performance of your system and staff, while finding opportunities to improve efficiency.
About RF Technologies:
RFT is a turn-key manufacturer and provider of life safety solutions for the senior living, healthcare, education, and hospitality markets. With 10,000+ installations since their founding in 1987, RFT is a collaborative partner in designing custom-configured solutions that meet each customer’s needs and reduces their liabilities. The RFT family of solutions includes CODE ALERT call and wander management, SAFE PLACE® patient security and staff protection, HELP ALERT® staff duress, SENSATEC® fall management products and EXACTRACK® equipment location.







